Seborrheic dermatitis is a common skin condition caused by an overproduction of sebum, which can be exacerbated by a viral infection. The most common viruses that cause seborrheic dermatitis are the common cold and the flu, but other viruses, such as COVID-19 (coronavirus 2019), can also cause this condition.
If you suffered from seborrheic dermatitis, falling sick with COVID-19 can suppress your immune system, triggering a severe SD flare.
Let’s take a deep dive:
- Can COVID cause seborrheic dermatitis?
- COVID-19 infection and the skin in humans
- Can COVID affect my skin?
- How do viral infections affect seborrheic dermatitis?
- How does your immune system act after you recover from COVID-19?
- Am I more likely to develop COVID-19 as a result of having seborrheic dermatitis?
- To wrap up
Can COVID cause seborrheic dermatitis?
COVID and other viral infections cause temporary immunosuppression, leading to flares of seborrheic dermatitis. If you already suffer from SD, contacting COVID can potentially trigger a severe flare.
In some cases, COVID can cause seborrheic dermatitis to occur suddenly for the first time. If your SD was caused by a COVID infection, it’s too early to tell if seborrheic dermatitis will be an ongoing chronic disease you have to deal with years into the future. I suspect you already have a predisposition to SD. Maybe you already had unrecognized mild SD and COVID made it much worse.
In my case, I was already struggling with progressively severe seborrheic dermatitis of the face and neck for 4-5 months before I had the misfortune of contacting COVID.
In the acute phase of COVID (the first 5 days), I had the usual flu symptoms, muscle aches and fever. There was no sign of a skin rash or any other skin lesions. However, when my initial symptoms resolved, my seborrheic dermatitis rash on my face, neck and scalp flared in a big way.
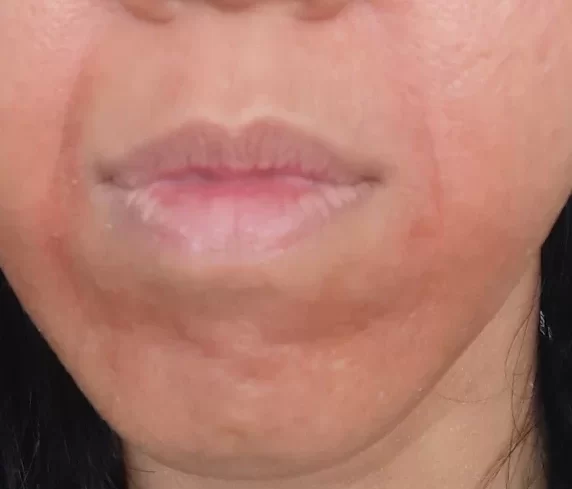
The rash flared every day for 4 days, getting worse as the days went by. It affected my whole face, including my eyelids and outer ear canal. My neck, scalp and armpits were also affected. I even got dry and itchy eyes! The rash was red and itchy, and fissures formed around my mouth. It burned to high heaven whenever I washed my face or put a cream on.
The only face cream that didn’t burn as much was MooGoo Scalp Cream:
After the initial cytokine thunderstorm, there was another week of extreme sensitivity to almost any and every trigger, then my skin started to slowly but surely recover. The recovery period took 3 weeks for me. In that time, I still got ‘mini-flares’.
COVID-19 infection and the skin in humans
There is a lot of information out there about COVID-19. What it is, how it’s spread, and the best ways to protect yourself from infection. But one thing that’s not always clear is how the virus affects the skin.
One potential complication of this virus is that it can disrupt the epidermal barrier. Multiple skin manifestations hae been described in people affected by COVID. These include rashes, blisters, hives, seborrheic dermatitis and many others.
It is now widely accepted that the complications of COVID occur due to our body’s immune response to the COVID virus rather than a direct effect of the virus itself. These same cytokines are found in high levels in skin affected by SD. So it makes sense that as we recover from COVID, that’s when our SD will flare up like a burning bush.
Can COVID affect my skin?
Yes, COVID can definitely affect your skin! In fact, it can cause a wide variety of skin problems. Some of the most common are exacerbations of eczema. Often times, COVID causes peeling skin which can occur for a few weeks after the initial symptoms go away.
COVID also produces a widespread rash called a viral exanthem. It’s usually not too severe but can be quite itchy.
How do viral infections affect seborrheic dermatitis?
HIV is a viral infection that is commonly associated with seborrheic dermatitis. People with HIV might present with a more severe, atypical form of SD that can be resistant to treatment. There is no evidence that viral infections like the flu virus and COVID-19 make underlying skin conditions, including eczema and seborrheic dermatitis worse.
However, there is no evidence that viral infections don’t worsen dermatitis either. I think there is just a lack of studies looking at this link.
Viral infections can cause temporary immunosuppression and lymphopenia, similar to HIV. Viruses can also trigger a cytokine storm in our body, which can exacerbate SD.
How does your immune system act after you recover from COVID-19?
The immune system is still in a recovery mode after someone has recovered from COVID-19. It can take weeks or even months for the immune system to return to its normal function. During this time, it is important to take steps to help support the immune system so that it can continue to function properly.
There is still much to learn about the immune system and how it behaves after you recover from COVID-19.
Am I more likely to develop COVID-19 as a result of having seborrheic dermatitis?
There is no evidence to suggest that people with SD are more likely to develop COVID-19 or to experience a more severe form of the condition if you do develop it.
However, if you are immunosuppressed from other illnesses, then you’re at risk for moderate to severe COVID.
To wrap up
Post-COVID seborrheic dermatitis happens. If your SD flared after a COVID infection, don’t worry. Concentrate on rebuilding your immune system. Your SD rash will slowly improve over a few weeks.
 Check it out on Amazon
Check it out on Amazon
Pingback: What triggers seborrheic dermatitis?
Pingback: Why did I suddenly get seborrheic dermatitis?
Pingback: Does depression cause seborrheic dermatitis?
Pingback: why does seborrheic dermatitis happen